
Motion Analysis Centers
For some children, coordinating complex movements like running with their friends, picking up a pencil, or throwing a baseball can be uncomfortable, difficult or even impossible.
As a child grows and develops, so does their ability to move. When a child has a condition that changes typical development and makes movement difficult, advanced diagnostic techniques may be necessary to understand fully what’s causing the movement problem. Motion analysis can help us understand the movement of children with neuromuscular, acquired or congenital disorders and develop an appropriate plan based on what we learn.
The specialists at our motion analysis centers (MACs) provide information used to drive treatment decisions for patients with a wide range of conditions. This includes cerebral palsy, brachial plexus (Erb's palsy), scoliosis, spinal cord injury, arthrogryposis, clubfoot, muscular dystrophy and spina bifida.
Our technology, which includes some of the same technical special effects used in movies and video games, collects information that provides Shriners Children’s care teams with guidance for a child's surgery, braces and/or rehabilitation.
During a session, we might explore your child’s ability to walk, run, bend and twist, and even how they swing their arms. Our state-of-the-art motion capture camera system records your child’s movements through the reflective markers we place on their body. Once we analyze the information we collect, we’ll partner with your child’s Shriners Children’s care team to recommend a care plan, making changes that can reduce their pain or discomfort and ultimately make it easier to do those things that are important to them.
How is Motion Analysis Information Used?
- Guide decisions regarding surgery, bracing/orthotics, medical management and/or rehabilitation
- Better evaluate the outcomes of treatment (surgery, braces, etc.) on a child’s mobility and their ability to perform daily tasks
- Provide a clearer understanding of how a child uses their walking aids or wheelchair
- Detect subtle changes over time that, if addressed early, may prevent or minimize additional loss of function
Our network of Shriners Children’s MACs is the largest of its kind in the world. Through regular communication between our MAC locations, we share information, data and knowledge, which helps all of the children we treat.
A visit to a Shriners Children’s motion analysis center can help unravel the mystery and put your child on the path to reaching their goals and discovering their full potential. Read on, to learn more about the services our MACs offer and how to prepare for a visit to one of our centers.
Specific treatments and services may vary by location. Please contact a specific location for more information.
During a motion analysis test, our team collects information related to your child’s movement, their muscle activity and the forces their body uses to move.
All of our locations perform the following motion analysis tests:
- Gait analysis (kinematics/kinetics)
- Foot pressure analysis
- Electromyography
- Joint range of motion and limb alignment
- Strength
- Motor control
In addition, some MACs perform the following specialized testing:
- Sports testing
- Spine motion analysis
- Wheelchair analysis (propulsion testing)
- Upper extremity kinematic analysis
- Jump landing analysis
- Running analysis
- Hip motion analysis
- Static balance analysis
- Oxygen consumption
All of the children seen at our MACs are Shriners Children’s patients referred to us by their Shriners Children’s doctor. Many children visit a MAC the same day as their appointment with their doctor, which means no lost time scheduling another appointment or driving somewhere else. A motion analysis study, which you might also hear called a gait study, walking study or walking test, can take between 90 minutes and several hours, depending on what's being evaluated.
Preparing for Your First MAC Appointment
Before you come in for your appointment, we’ll go over the specifics with you, but here are a few things that will help you and your child get ready.
- Clean your child's arms, feet and legs the morning of the appointment.
- Do not apply lotion to your child’s body on the day of testing.
- Bring elastic waistband shorts and a T-shirt to wear during the evaluation.
- Girls should also bring a non-racerback sports bra and a camisole top that does not cover the upper back or shoulders.
- Bring any orthotic braces your child wears (or no longer wears) and any shoes they wear with or without braces.
- Bring any assistive devices such as walkers, crutches and/or gait trainers.
- Bring glasses and hearing aids if your child uses them.
Things to Think About Before Your Visit
Does your child play a sport or an instrument? What do they want to do? It’s extremely helpful for us to hear from those who interact with your child when they are, or are not, wearing or using a device. What do they do well? What do they have trouble with? Gather some notes and your questions, and bring them with you.
What happens during a motion analysis evaluation?
Using infrared cameras mounted around a large room, a child’s movements are tracked and displayed virtually as they walk down a runway and walk across or stand on a special force platform. The information gathered in this exercise is translated to 3D animation, which allows the team to analyze your child’s movement.
This process is not painful and is often fun. In fact, many of the children who visit one of our nationally recognized MACs say these are some of the most fun and least scary tests they’ve taken.
Some test specifics:
- Specialized cameras capture the movements of sticky markers we attach to your child’s feet, legs and trunk (kinematics).
- Electromyograph electrodes are placed on your child's legs to evaluate their muscle activity (EMG).
- Platforms recessed into the floor measure forces acting on the body as your child walks (kinetics).
- A special walkway measures the pressure under the surface of your child’s foot while they walk (pedobarograph).
- High-definition video cameras record how your child walks, bends, raises his or her arms and legs and completes other tasks as needed.
- Metabolic testing measures how much energy your child expends while walking.
The Follow-Up
After the test, the information we’ve gathered is reviewed by a multidisciplinary team of specialists, including orthopedic surgeons, an engineer, a kinesiologist, and a physical therapist. Once the results have been reviewed, you'll return with your child and discuss next steps with his or her care team. Some children return for additional MAC appointments, perhaps after surgery, after rehabilitation, after wearing a brace, etc., to have the test repeated and understand how they are progressing and adjust their treatment plan if needed.
The Shriners Children's Motion Analysis Network (SMACnet) is a group of Shriners Children's physicians, therapists, engineers, kinesiologists and technicians who work together to improve the clinical, research and educational activities in Shriners Children’s MACs.
The partnership and communication between SMACnet members allows us to develop innovative solutions that directly impact and increase our ability to treat complex movement disorders in children. Each MAC sees hundreds of patients per year, and with each child we assess, we collect, organize and store data. Recently, SMACnet established a combined patient database. One of the largest MAC patient databases in the world, the anonymous data from all of the patients that visit the MAC will be used together to improve treatment for children across Shriners Children's and often outside our healthcare system.
Research by Shriners MACs
Research in our MACs helps us better understand normal motion, which means we are also able to increase our understanding of uncommon motion.
As leaders in the field of motion analysis, members of SMACnet publish multiple peer-reviewed articles each year. Below are a few of the areas we’re currently involved in, with links to articles we've written about particular subjects.
Measuring Foot Motion
We've pioneered several different approaches for measuring foot motion. These new techniques help us better understand how the foot moves and the possible interventions that may improve a child's ability to walk.
- A musculoskeletal foot model for clinical gait analysis (Journal of Biomechanics, 2010)
- Segmental foot and ankle kinematic differences between rectus, planus, and cavus foot types (Journal of Biomechanics, 2019)
- Center of pressure metrics derived from spatially registered typically developing data (Gait & Posture, 2020)
Effects of Early Mobilization on Outcomes after Cerebral Palsy Surgery
This research shows how starting rehabilitation within the first few days of multilevel cerebral palsy surgery, instead of waiting three to six weeks, can have a significant, positive impact on a child. Within the first month after surgery, improvements seen included restoring a child’s participation in daily activities, including walking and returning to school.
Evaluating Surgical Interventions that Improve Mobility
SMACnet has published many scientific papers exploring the biomechanics (structure, function and motion) of gait and surgical outcomes.
- Femoral anteversion assessment: Comparison of physical examination, gait analysis, and EOS biplanar radiography (Gait & Posture, 2018)
- Midstance hamstring length is a better indicator for hamstring lengthening procedures than initial contact length (Gait & Posture, 2020)
- Patella Alta in Ambulatory Children With Cerebral Palsy: Prevalence and Functional Significance (Journal of Pediatric Orthopedics, 2020)
- Utilization and efficacy of computational gait analysis for hamstring lengthening surgery (Gait & Posture, 2016)
Upper Extremity Motion
In addition to walking, some of our motion analysis labs have been quantifying upper extremity motion. SMACnet work in this area has included exploring upper extremity motion in cerebral palsy, spinal cord injury, scoliosis and brachial plexus (Erb's palsy) injuries.
- Upper extremity biomechanics of children with spinal cord injury during wheelchair mobility (Annual International Conference of the IEEE Engineering in Medicine and Biology Society, 2014)
- Analysis of Shoulder Complex Function After Posterior Spinal Fusion in Adolescents With Idiopathic Scoliosis (Journal of Pediatric Orthopedics, 2019)
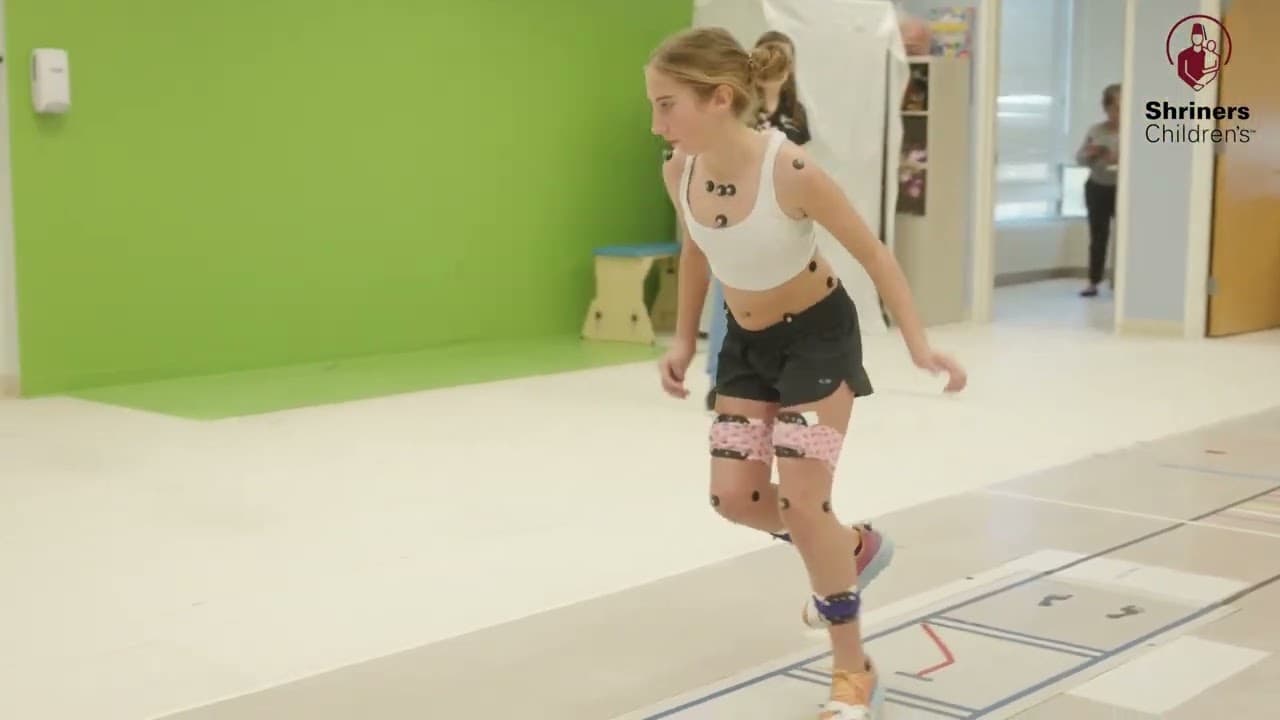
Our motion analysis centers combine state-of-the-art technologies with highly qualified and deeply caring orthopedic specialists. Their work leads to exceptional care for children with conditions that affect their movement.

Pediatric Orthopedics: Specialized Care for Growing Bones
Conditions We Support
View All
Clubfoot / Club feet

Toe-Walking

Intoeing

Out Toeing

Pes Planus / Pes Planovalgus

Spinal Cord Injury

Congenital Neuromuscular Disorders

Scoliosis

